How to Recognize Thrush Symptoms (Oropharyngeal Candidiasis)
What is thrush?
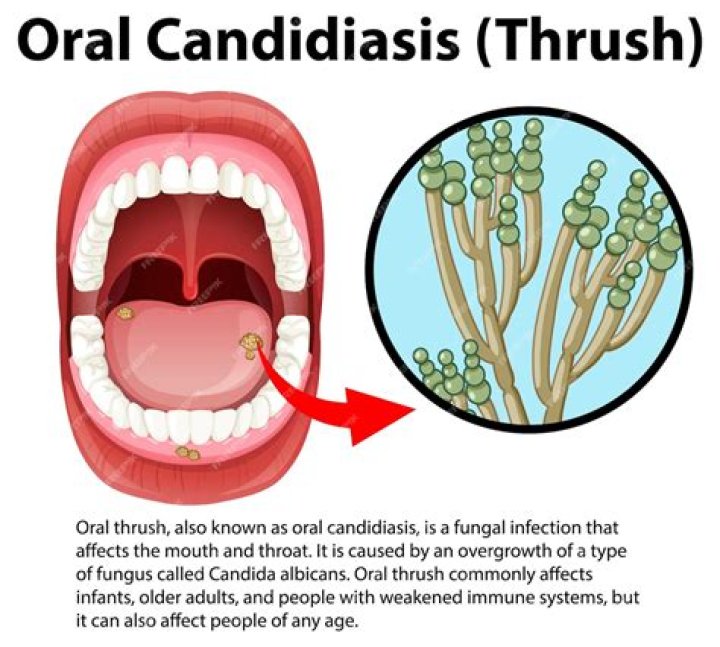
Thrush is a fungal (yeast) infection that can grow in your mouth, throat and other parts of your body. In your mouth thrush appears as a growth that can look like cottage cheese – white, raised lesions on your tongue and cheeks. The condition can quickly become irritated and cause mouth pain and redness.
Thrush is caused by the overgrowth of a type of fungus called Candida. Mouth and throat thrush is called oropharyngeal candidiasis.
A thrush infection is annoying but it’s generally a minor problem for healthy people and will clear up in a few weeks with antifungal treatment.
Who can get thrush and is it contagious (pass from person to person)?
While thrush can affect anyone, babies under 1 month old, toddlers, older adults and people with weakened immune systems (where symptoms can be harder to control) are at more risk. Thrush in the esophagus (swallowing tube) is one of the more common infections in people with HIV/AIDS.
Thrush can be contagious to those at risk (like people with weakened immune systems or are taking certain medications). In healthy people, it’s unusual for it to be passed on through kissing or other close contacts. In most cases, thrush isn’t considered particularly contagious but it can be transmitted.
If you’re worried about getting thrush from another person who has it, avoid coming into contact with their saliva (spit). It’s smart to wash your hands as often as possible if you’re near someone who has thrush.
Why is thrush a concern during breastfeeding?
Because infants are more at risk, getting or giving thrush during breastfeeding is a worry with many moms. It’s a common breastfeeding problem, and in some cases treatment can be tricky.
Babies with thrush can pass the infection to their mothers. When the infection in a baby’s mouth leads to sore throat and pain, they cry and are irritable during feeding. Mothers (especially if they’re taking antibiotics) may also develop thrush infections around the breasts and nipples and transmit it to their babies.
When both mom and baby develop thrush they should be treated for the condition at the same time to prevent an ongoing exchange of the infection.
What causes thrush?
Most people have small amounts of the Candida fungus in the mouth, digestive tract and skin. They are normally kept in check by other bacteria and microorganisms in the body. When illnesses, stress, or medications disturb this balance, the fungus grows out of control and causes thrush.
Medications that can make yeast flourish and cause infection include:
Candida infection is more likely to develop with:
- Uncontrolled diabetes.
- HIV infection.
- Cancer.
- Dry mouth.
- Pregnancy (caused by the hormonal changes that occur with pregnancy).
- Smoking.
- Wearing dentures that don’t fit well.
What are the symptoms of thrush?
Thrush usually develops suddenly. A common sign is the presence of those creamy white, slightly raised lesions in your mouth — usually on your tongue or inner cheeks. They can also be seen on the roof of your mouth, gums, tonsils or back of your throat. Other symptoms may be:
- Redness and soreness inside and at the corners of your mouth.
- Loss of ability to taste.
- Cottony feeling in your mouth.
The lesions can hurt and may bleed a little when you scrape them or brush your teeth. In severe cases, the lesions can spread into your esophagus and cause:
- Pain or difficulty swallowing.
- A feeling that food gets stuck in the throat or mid-chest area.
- Fever, if the infection spreads beyond the esophagus.
Thrush can spread to other parts of the body, including the lungs, liver and skin. This happens more often in people with cancer, HIV or other conditions that weaken the immune system.
Last reviewed by a Cleveland Clinic medical professional on 10/22/2019.
References
- The American Academy of Oral Medicine. Oral Yeast Infections (Thrush or Candidiasis) Accessed 11/5/2019.
- Centers for Disease Control and Prevention. Oropharyngeal/Esophageal Candidiasis (“Thrush”) Accessed 11/5/2019.
- Akpan A, Morgan R. Oral candidiasis. Postgraduate Medical Journal. 2002;78(922):455-459. doi:10.1136/pmj.78.922.455. ncbi.nlm.nih.gov Accessed 11/5/2019.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Oropharyngeal candidiasis or oral thrush is a medical condition caused by fungus overgrowth in the throat and mouth. This fungus is usually present in the digestive tract, mouth, and skin of all healthy people. It is generally kept in balance by the body’s healthy bacteria and immune system. When this balance is disturbed, it results in an overgrowth of this fungus, causing thrush.
Read the blog to learn more about oral thrush symptoms and the available treatments.
What Causes Oral Thrush in Adults?
Oral thrush is the result of an overgrowth of the fungus named Candida albicans in the mouth or throat. The excessive growth of this fungus is triggered due to different factors such as pregnancy, illness, new medications, or variations in the immune system.
Oral Thrush Treatment
Treatment of thrush mostly depends on its cause and severity. Doctors usually prescribe antifungal medications like lozenges or a topical oral suspension for treating thrush. However, for patients with compromised immune system, antifungals are administered either orally or intravenously.
Home Remedies for Oral Thrush
Some useful home remedies for oral thrush include:
- Practicing good oral hygiene
- Disinfecting dentures
- Warm salt water rinse
- Using nursing pads
- Eating soft, easy-to-swallow foods
Is Oral Thrush Contagious?
Usually, thrush is non-contagious, but it may occasionally pass from one person to another. For example, a breast-feeding baby with thrush may pass it by contact with the mother’s breast. Thrush infection is considered to be highly dependent on your immune system’s strength.
How Long Does Oral Thrush Last Without Treatment?
Very mild cases of thrush clear up with the use of over-the-counter solutions. If appropriately treated, it will go away in about two weeks. However, if left untreated, severe thrush can cause other severe systemic candida infections. For example, if you have an impaired immune system, thrush can spread to other areas of your body, such as the esophagus. Also, there is a chance of recurrence if it is left untreated.
If you experience symptoms of oral thrush, contact our Shoreline dentists or Milton dentists today for a consultation.
- Candida
- Causes of candidiasis
- Signs and symptoms of candidiasis
- Oropharyngeal / oesophageal candidiasis (oral thrush)
- Genital Candidiasis / vulvovaginal candidiasis (VVC) / Candidal vulvovaginitis
- Cutaneous Candidiasis / Candida Skin Infection
- Invasive candidiasis
- What is Candida die-off?
- Candida Diet and Outlook for the infection
Candida infection that involves the mouth, throat and/or oesophagus is referred to as oropharyngeal or oesophageal candidiasis or thrush.
Causes of oral thrush
Oral thrush occurs when certain medications (like antibiotics or corticosteroids) are taken or the immune system is weakened due to illness. These medications as well as certain health conditions disturb the natural balance of ‘healthy bacteria’ in the body which leads to the multiplication of Candida 14 . When this growth remains unchecked, an infection (candidiasis) occurs and leads to the development of various symptoms associated with oral thrush.
Oral thrush symptoms
What does oral thrush look like?
Oral thrush is generally easily identified by a thick, white coating on the tongue and white patches / plaques on the insides of the cheeks and throat. As one descends down the throat and into the gastrointestinal tract (generally only visible when using an endoscope), the patches continue, as is evident in the images below.
From left to right: Oral candidiasis apparent on the tongue, back of the throat, and the oesophagus.
Other symptoms may include:
- Soreness or redness in the areas affected
- Difficulty in swallowing
- Painful sores on the sides of the mouth that result in the corners cracking due to the build-up of microorganisms (this is known as angular cheilitis) – these sores often cause a burning sensation in the affected area
- Nausea
- Vomiting
- Weight loss
If you are experiencing any of these symptoms, it is advised that you see your doctor for treatment. The earlier treatment begins, the better the outlook.
Who is at risk of developing oral candidiasis?
Babies, toddlers, the elderly and people who suffer from a weakened immune system are most at risk of experiencing oral candidiasis (oral thrush). These infections are uncommon in healthy adults.
Other factors that are associated with the development of oesophageal and oral candidiasis, these include:
- Broad-spectrum antibiotic use – these are antibiotics that work against a large range of bacteria, including the healthy bacteria that keep Candida growth in check.
- Corticosteroid use (including inhaled corticosteroids for conditions like asthma)
- Diabetes that is poorly managed
- Poorly fitted dentures
- Cancer treatments – These include radiation and chemotherapy as these treatment methods have an adverse impact on the immune system
- HIV/AIDS infection
- Organ transplantation
Can oral candidiasis be prevented?
The development of oral thrush depends on the strength of one’s immune system, this is why babies, the elderly and the immunocompromised are often most affected. Practising good oral hygiene helps to prevent oral thrush from occurring.
Some studies show that mouthwash containing chlorhexidine (CHX) can aid in preventing oral thrush 15,16 . Those who use an inhaler for the administration of corticosteroids (asthma medication), can benefit from washing their mouth out with mouthwash or even water after using their inhaler.
Diagnosis of oral thrush
An oral thrush infection will be diagnosed based on visible symptoms. The treating doctor may also scrape off some of the affected area in order for it to be examined. This procedure is quick and painless and allows for the sample of the infected area to be analysed and tested for the presence of fungal infections.
A culture test using a cotton swab can also be performed, however, due to the fact that Candida organisms occur naturally in the mouth, if the culture test is positive, this is not enough evidence to make an accurate diagnosis of infection (candidiasis).
Treatment of oral thrush and outcome
Antifungal medication is typically prescribed for oral thrush 16 . The duration and type of treatment will be dependent on the infection’s severity, as well as various factors regarding the sufferer such as their age and immune system status.
Topical treatments including nystatin suspension and clotrimazole troches are often used in the treatment of oral thrush. Antifungal medication that is systemic (i.e. drugs that act through the entire body), such as itraconazole or fluconazole, are sometimes necessary when oropharyngeal infections do not respond to other medications.
Itraconazole or intravenous fluconazole are common treatments for Candida esophagitis. In more severe cases of oesophageal candidiasis that do not respond to antifungal medications, a treatment containing amphotericin B may be used. This form of treatment will injure the membranes of the fungal cell, making it more permeable for other medications to treat and eliminate.
References
14. Agrawal A, Singh A, Verma R, Murari A. Oral candidiasis: An overview. Journal of Oral and Maxillofacial Pathology . 2014;18(4):81. doi:10.4103/0973-029x.141325
15. Scheibler E, Garcia M, Medina da Silva R, Figueiredo M, Salum F, Cherubini K. Use of nystatin and chlorhexidine in oral medicine: Properties, indications and pitfalls with focus on geriatric patients. Gerodontology. 2017;34(3):291-298. doi:10.1111/ger.12278
16. Oral thrush: Prevention during cancer treatment. Ncbi.nlm.nih.gov. Published 2006. Accessed May 22, 2019.
17. Patil S, Rao R, Majumdar B, Anil S. Clinical Appearance of Oral Candida Infection and Therapeutic Strategies. Front Microbiol. 2015;6.doi:10.3389/fmicb.2015.01391
Medically reviewed by Drugs.com. Last updated on Feb 3, 2020.
- Overview
- Aftercare Instructions
- Ambulatory Care
- En Español
WHAT YOU NEED TO KNOW:
What is oral candidiasis?
Oral candidiasis, or thrush, is a fungal infection that affects the inside of your mouth.
What causes oral candidiasis?
Oral candidiasis is caused by a type of fungus called Candida. Fungi are normally found in your mouth. When there are too many fungi, it can cause an infection. Babies and the elderly are at higher risk because their immune systems are not as strong. Newborn babies may get thrush if the mother had vaginal candidiasis during delivery. The following may increase your risk of oral candidiasis:
- Medical conditions that suppress your immune system, such as diabetes, cancer, or HIV and AIDS
- Medicines, such as antibiotics, steroids, or chemotherapy
- Radiation therapy to the head and neck
- Dry mouth
- Smoking
- Dentures
What are the signs and symptoms of oral candidiasis?
- White or whitish-yellow patches in the mouth that look like milk curds
- Redness or bleeding under the patches
- Sore and painful mouth, with cracking or tearing on the corners
- Bright red tongue that may feel like it is burning
- Trouble swallowing and tasting
- Swelling under dentures
How is oral candidiasis diagnosed?
Your healthcare provider will ask about your medical history. He will ask when your signs and symptoms started. He will examine the inside of your mouth and the area around your mouth. Your healthcare provider will also rub a cotton swab on one of the patches and check it under a microscope.
How is oral candidiasis treated?
Antifungal medicine helps kill the fungus that caused your oral candidiasis. This medicine may be a pill or a solution that you gargle. Remove dentures before you gargle.
How can I help to prevent oral candidiasis?
Brush your teeth, gums, and tongue after you eat and before you go to sleep. Use a toothbrush with soft bristles. See your dentist for regular exams. Remove your dentures when you sleep, or at least 6 hours each day. Clean your dentures and soak them in denture cleaner. Let them air dry after soaking.
When should I seek immediate care?
- You have trouble swallowing and your jaw and neck are stiff.
- You are dizzy, thirsty, or have a dry mouth.
- You are urinating little or not at all.
- You cannot eat or drink because of the pain.
When should I contact my healthcare provider?
- You have a fever.
- You have nausea, vomiting, or diarrhea.
- Your signs and symptoms get worse, even after treatment.
- You have questions or concerns about your condition or care.
Care Agreement
© Copyright IBM Corporation 2020 Information is for End User’s use only and may not be sold, redistributed or otherwise used for commercial purposes. All illustrations and images included in CareNotes® are the copyrighted property of A.D.A.M., Inc. or IBM Watson Health
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
In this Article
In this Article
In this Article
- Thrush (Oropharyngeal Candidiasis)
- Genital Yeast Infection (Genital Candidiasis)
- Diaper Rash From Yeast Infection
- Invasive Candidiasis
There are many kinds of fungus that live in the human body. One type is called candida. It’s a type of yeast that normally lives in small amounts in places like your mouth and belly, or on your skin without causing any problems. But when the environment is right, the yeast can multiply and grow out of control.
The infection it causes is called candidiasis. There are several different types of it. Most can be easily treated with over-the-counter or prescription medications.
Thrush (Oropharyngeal Candidiasis)
When the candida yeast spreads in the mouth and throat, it can cause an infection called thrush. It’s most common in newborns, the elderly and people with weakened immune systems. Also more likely to get it are adults who:
- Are being treated for cancer
- Take medications like corticosteroids and wide-spectrum antibiotics
- Wear dentures
- Have diabetes
The symptoms include:
- White or yellow patches on the tongue, lips, gums, roof of mouth, and inner cheeks
- Redness or soreness in the mouth and throat
- Cracking at the corners of the mouth
- Pain when swallowing, if it spreads to the throat
Thrush is treated with antifungal medicines like nystatin, clotrimazole, and fluconazole. Rinsing the mouth with chlorhexidine (CHX) mouthwash may help prevent infections in people with weakened immune systems.
Genital Yeast Infection (Genital Candidiasis)
Three out of four adult women will get at least one yeast infection during their lifetime. This occurs when too much yeast grows in the vagina. (Men also can get a genital yeast infection, but it’s much less common).
A yeast infection typically happens when the balance in the vagina changes. This can be caused by pregnancy, diabetes, use of some medicines, lubricants, or spermicides, or a weakened immune system. Occasionally, the infection can be passed from person to person during sex.
The symptoms include:
- Extreme itchiness in the vagina
- Redness and swelling of the vagina and vulva (the outer part of the female genitals)
- Pain and burning when you pee
- Discomfort during sex
- A thick, white “cottage cheese” discharge from the vagina
A man with a yeast infection may have an itchy rash on his penis.
Continued
Because the symptoms in women can be similar to other infections like bacterial vaginosis (bacterial overgrowth in the vagina) and sexually transmitted diseases, it’s important to visit your doctor.
Most times, an over-the-counter antifungal suppository, tablet, or cream will knock out the infection. Your doctor might also prescribe a single dose of a prescription antifungal medicine like fluconazole. Tell your doctor if you get yeast infections more than four times a year. She may recommend regular doses of antifungal medication over several months to fight the repeated infections.
Diaper Rash From Yeast Infection
Though diaper rashes are usually caused by leaving a wet or soiled diaper on too long, once your baby’s skin is irritated, infection is more likely. If his diaper rash isn’t going away, check to see if his bottom is red and sensitive, and if there’s a raised red border around the sores. If so, have your pediatrician check for candidiasis. It can be treated with an antifungal cream.
Keeping your baby’s bottom clean and dry is a good start to help prevent diaper rash and candidiasis.
Invasive Candidiasis
If candida yeast enters the bloodstream (usually through medical equipment or devices), it can travel to the heart, brain, blood, eyes, and bones. This can cause a serious, life-threatening infection.
This happens most often to people who have recently been admitted to a hospital or live in a health care facility, such as a nursing home. Like other types of yeast infections, if you have diabetes, a weakened immune system, kidney failure, or are on antibiotics, your chances of getting it are greater.
The symptoms include fever and chills. Since it’s likely a person with this infection is already sick with another condition, it can be hard to diagnose.
Invasive candidiasis is treated with an oral or intravenous dose of antifungal medication. If you are having surgery and have higher odds of a yeast infection, your doctor might prescribe a series of antifungal medicines before the procedure.
Sources
CDC: “Candidiasis,” “Oropharyngeal/Esophageal Candidiasis,” “Genital/vulvovaginal candidiasis (VVC),” “Invasive Candidiasis.”
HealthyChildren.org: “Thrush and Other Candida Infections,” “Diaper Rash.”
American Congress of Obstetricians and Gynecologists: “Vaginitis.”
Affiliation
- 1 Division of Medicine, University of Crete, Heraklion, Greece.
- PMID: 9709877
- DOI: 10.1086/514653
- Search in PubMed
- Search in NLM Catalog
- Add to Search
Authors
Affiliation
- 1 Division of Medicine, University of Crete, Heraklion, Greece.
- PMID: 9709877
- DOI: 10.1086/514653
Abstract
The present study was designed to determine the frequency of candidal esophagitis in cancer patients with oral thrush. Patients with clinically and microbiologically diagnosed oral candidiasis were evaluated by endoscopy for concurrent esophageal candidiasis. Esophageal involvement was documented by mucosal lesions, microbiological findings of candidal infection in smears of brushing material, positive cultures of brushing material, and histological evidence of mucosal invasion by the yeast. For 21 of the 22 patients studied, there were endoscopic and microbiological findings of candidal esophagitis. Cultures of the brushing material from all 22 patients were positive, while histological evidence was found for 14 patients. Only 10 of the patients had mild esophageal symptoms. It is concluded that oral thrush represents a reliable marker for esophageal candidiasis in patients with cancer. Routine endoscopy is not necessary to confirm the diagnosis; this procedure should be reserved for patients with persistent thrush and symptoms despite antifungal therapy.
Background Oropharyngeal candidiasis (thrush) occurs commonly in seriously ill and dying patients.
Risk Factors Risk factors include a) either acquired (HIV-AIDS) or drug-induced (chemotherapy, inhaled or systemic glucocorticoids) defects of cell-mediated immunity; b) disruption of the oropharyngeal mucosa by cytotoxic chemotherapy (See Fast Fact #121) or radiation that includes the oropharynx; c) xerostomia (dry mouth) from any cause; d) diabetes mellitus; e) recent antibiotic use; f) dentures; g) advanced age; h) poor oral hygiene; and i) poor nutritional status.
Diagnosis Thrush is often asymptomatic but can lead to oral pain, oropharyngeal dysphagia, halitosis, alterations in taste, diminished appetite, and reduced oral intake. Thrush may or may not be present in cases of esophageal candidiasis, which presents as odynophagia and esophageal dysphagia. Most cases of thrush are caused by Candida albicans; C. krusei, glabrata, or tropicalis are sometimes implicated in AIDS and cancer patients. Diagnosis is made on clinical findings: white or yellow, cottage-cheese like plaques on the buccal mucosa, tongue, or palate. The plaques are easily removed, leaving a red or bleeding and often painful base. A less common presentation – seen in AIDS or in patients with poorly fitting dentures – involves red, edematous, and sometimes eroded mucosal lesions, but without plaques. If diagnostic doubt exists, confirmation can be made by KOH staining a wet-prep of a plaque scraping, revealing pseudohyphal Candidal forms. Culture is not recommended, as Candida species are common colonizers of the mouth.
Treatment The decision to treat thrush should be based on the patient’s overall condition, prognosis, symptoms, and goals of care. Treatments include either systemic or topical anti-fungal drugs. All regimens should be continued for 7-14 days. Meticulous attention to denture cleaning, if applicable, is important to prevent recurrence. If esophageal candidiasis is suspected, systemic therapy is necessary as topical treatment is ineffective.
Topical drugs are the most commonly used but problems can occur due to patient objections to taste and compliance with multiple daily dosing.
- Nystatin suspension (“swish and swallow”) is dosed as 200,000-500,000 Units 4 – 5 times a day. It is substantially less effective in immunocompromised patients than the azole anti-fungals (30-50% vs 70-90% effective) and should not be used in this population.
- Clotrimazole (10 mg troches 5 times a day) is nearly as effective as the systemic azole anti-fungals; however, it is associated with a higher recurrence rate of thrush.
- Systemic drugs are more effective than the topicals. However they are more expensive and have significant drug-drug interactions—especially with macrolide antibiotics, anticonvulsants, benzodiazepines, methadone, and coumadin.
- Fluconazole is the systemic treatment of choice; it is more effective with fewer drug interactions than ketoconazole. Many dosing regimens have been described: 200 mg once, then 100 mg daily for 14 days total is most commonly used.
- Itraconazole suspension (200 mg daily) is an alternative to fluconazole. It is better absorbed and more effective than itraconazole capsules.
- Note: Fluconazole resistant candidiasis is rare, but becoming more common. Itraconazole, IV or oral amphotericin, voriconazole, and caspofungin have all been used with success.
Recommendations Clotrimazole troches are a reasonable first line therapy for patients in the palliative care setting if the troches are tolerable and 5 times a day dosing is acceptable. If not, and/or if the patient has problems with recurrent thrush, fluconazole should be used.
References
- Willberg P, Hjermstad MJ, Ottesen S, et al. Oral health is an important issue in end-of-life cancer care. Support Care Cancer. 2012; 20:3115-3122.
- Pienaar ED, Young T, Holmes H. Interventions for the prevention and management of oropharyngeal candidiasis associated with HIV infection in adults and children. Cochrane Database of Systemic Reviews. 2010, Issue 11. Art. No.: CD003940. DOI: 10.1002/14651858.CD003940.pub3.
- Davies AN, Brailsford SR, Beighton D, et al. Oral Candidosis in Community-Based Patients with Advanced Cancer. J Pain and Symptom Management. 2008; 35(5):508-514.
- Wiseman M. The Treatment of Oral Problems in the Palliative Patient. J Can Dent Assoc. 2006; 72(5):453-8.
- Davies AN, Brailsford SR, Beighton D. Oral candidosis in patients with advanced cancer. Oral Oncology. 2006; 42:698-702.
- Pappas PG, Kauffman CA, Andes D, et al. Clinical practice guidelines for the management of candidiasis: 2009 update by the Infectious Disease Society of America. Clin Infect Dis. 2009; 48:503-35.
Version History: This Fast Fact was originally edited by David E Weissman MD and published in December 2005. Copy-edited in April 2009. In September 2015 it was re-copy-edited with reference #6 was added and reflected in the text.
Fast Facts and Concepts are edited by Sean Marks MD (Medical College of Wisconsin) and associate editor Drew A Rosielle MD (University of Minnesota Medical School), with the generous support of a volunteer peer-review editorial board, and are made available online by the Palliative Care Network of Wisconsin (PCNOW); the authors of each individual Fast Fact are solely responsible for that Fast Fact’s content. The full set of Fast Facts are available at Palliative Care Network of Wisconsin with contact information, and how to reference Fast Facts.
Copyright: All Fast Facts and Concepts are published under a Creative Commons Attribution-NonCommercial 4.0 International Copyright (). Fast Facts can only be copied and distributed for non-commercial, educational purposes. If you adapt or distribute a Fast Fact, let us know!
Disclaimer: Fast Facts and Concepts provide educational information for health care professionals. This information is not medical advice. Fast Facts are not continually updated, and new safety information may emerge after a Fast Fact is published. Health care providers should always exercise their own independent clinical judgment and consult other relevant and up-to-date experts and resources. Some Fast Facts cite the use of a product in a dosage, for an indication, or in a manner other than that recommended in the product labeling. Accordingly, the official prescribing information should be consulted before any such product is used.
About oral thrush in adults
Oral thrush is a fungal infection of the mouth. It is not contagious and is usually successfully treated with antifungal medication.
It is also called oral candidosis (or candiasis) because it is caused by a group of yeasts called Candida.
Symptoms of oral thrush can include:
- white patches (plaques) in the mouth that can often be wiped off, leaving behind red areas that may bleed slightly
- loss of taste or an unpleasant taste in the mouth
- redness inside the mouth and throat
- cracks at the corners of the mouth
- a painful, burning sensation in the mouth
In some cases, the symptoms of oral thrush can make eating and drinking difficult.
When to seek medical advice
Speak to your GP if you develop symptoms of oral thrush. If left untreated, the symptoms will often persist and your mouth will continue to feel uncomfortable.
In severe cases that are left untreated, there is also a risk of the infection spreading further into your body, which can be serious.
Your GP will usually be able to diagnose oral thrush simply by examining your mouth. Sometimes they may also recommend blood tests to look for certain conditions associated with oral thrush, such as diabetes and nutritional deficiencies.
What causes oral thrush?
Low numbers of the fungus Candida are naturally found in the mouth and digestive system of most people. They don’t usually cause any problems, but can lead to oral thrush if they multiply.
There are a number of reasons why this may happen, including:
- taking a course of antibiotics, particularly over a long period or at a high dose
- taking inhaled corticosteroid medication for asthma
- wearing dentures (false teeth), particularly if they don’t fit properly
- having poor oral hygiene
- having a dry mouth, either because of a medical condition or a medication you are taking
- smoking
- having chemotherapy or radiotherapy to treat cancer
Babies, young children and elderly people are at a particularly high risk of developing oral thrush, as are people with certain underlying conditions, including diabetes, an iron deficiency or vitamin B12 deficiency, an underactive thyroid (hypothyroidism) and HIV.
As most people already have Candida fungi living in their mouth, oral thrush is not contagious. This means it cannot be passed to others.
Treating oral thrush
Oral thrush can usually be successfully treated with antifungal medicines. These usually come in the form of gels or liquid that you apply directly inside your mouth (topical medication), although tablets or capsules are sometimes used.
Topical medication will usually need to be used several times a day for around 7 to 14 days. Tablet or capsules are usually taken once daily.
These medications don’t often have side effects, although some can cause nausea (feeling sick), vomiting, bloating, abdominal (tummy) pain and diarrhoea.
If antibiotics or corticosteroids are thought to be causing your oral thrush, the medicine – or the way it is delivered – may need to be changed or the dosage reduced.
Preventing oral thrush
There are a number of things you can do to reduce your chances of developing oral thrush, including:
- rinsing your mouth after meals
- brushing your teeth twice a day with a toothpaste that contains fluoride and interdental cleaning (flossing) regularly
- visiting your dentist regularly for check-ups, even if you wear dentures or have no natural teeth
- removing your dentures every night, cleaning them with paste or soap and water before soaking them in a solution of water and denture-cleaning tablets
- brushing your gums, tongue and inside your mouth with a soft brush twice a day if you wear dentures or have no or few natural teeth
- visiting your dentist if your dentures do not fit properly
- stopping smoking if you smoke
- rinsing your mouth with water and spitting it out after using a corticosteroid inhaler, and using a spacer (a plastic cylinder that attaches to the inhaler) when you take your medicine
- ensuring that any underlying condition you have, such as diabetes, is well controlled
If you have a condition or are receiving treatment that could put you at a high risk of developing oral thrush, your doctor may recommend taking a course of antifungal medication to prevent this happening.
Candida is a naturally occurring fungus that everyone has on their body. Under certain conditions, some types of Candida can grow too fast and cause an infection to develop. This infection is called candidiasis, and it can affect the skin or nails specifically.
In this article, we explain what Candida is, the symptoms of candidiasis of the skin and nails, and how to treat and prevent this infection.
Share on Pinterest Candidiasis can develop in folds of the skin and places where there is moisture and warmth.
Candida is a yeast that is present on the skin and the mucous membranes, which line the inside of many of the structures in the body.
It is usually harmless, but if changes occur in the body to create the right environment, it can cause an infection.
There are about 150 types of Candida.
More than 20 types, including the most common species Candida albicans, can cause infections in humans. These infections can occur in the nails, skin, and mucous membranes throughout the body.
Candidiasis is an infection with Candida.
Many Candida infections are localized and only affect one part of the body. For example, cutaneous candidiasis affects the skin, while onychomycosis is an infection of the nails.
Chronic mucocutaneous candidiasis (CMC) refers to a group of disorders that feature persistent, debilitating, and recurrent infections of the skin, nails, and mucous membranes.
CMC results from an immunodeficiency problem, which occurs due to genetic factors.
Thrush, or oropharyngeal candidiasis, is another type of Candida infection, which affects the mouth or throat. It is also possible to have a Candida infection of the vagina, which people tend to refer to as a yeast infection.
Invasive candidiasis is a more severe condition that is different than candidiasis of the skin and nails because it is not localized. Invasive candidiasis can affect the blood, brain, eyes, and other organs in the body, and it can be life-threatening.
Candida thrives in a warm, humid environment, and a reduced immune response or other conditions can allow an infection to develop.
The following factors make infection more likely:
- hot or humid weather
- poor hygiene
- infrequent diaper or undergarment changes
- tight clothing that rubs
- synthetic fabric that does not breathe well
- antibiotics that alter the body’s natural Candida balance
- frequent exposure to irritating substances
- doing a job that involves spending time in the water
- having an inflammatory disease, such as psoriasis, that occurs in skin folds
- immunosuppression due to the use of corticosteroids or specific medications
- pregnancy
- health conditions that affect the immune system, such as diabetes and some hormonal conditions, including particular thyroid problems, Addison’s disease, and Cushing’s disease
Candidiasis affects the skin and nails differently.
In the skin
Candidiasis of the skin can lead to:
- redness
- rash
- scaling
- swelling
These symptoms often occur in areas of the body that are more difficult to keep dry and in places where skin touches skin.
Some examples of these sensitive areas include:
- in folds of skin
- under the breasts
- the groin
- the armpits
- the spaces between fingers and toes
- the foreskin of an uncircumcised penis
In some people, the infection can also affect the mouth and throat.
The infection tends to itch and feel uncomfortable, but treatment can relieve the symptoms.
In the nails
Candidiasis of the nails can result in the following symptoms in the fingernails or toenails:
- brittle, easily breakable, or splitting nails
- white, brown, or yellow discoloration
- debris collecting under the nail
- thinning nails with a dry, powdery surface
- the nail lifting up and becoming detached
- the nail splitting or crumbling
Without treatment, the affected nails can become thicker and more discolored.
This condition is not usually painful, but, if the infection progresses in the toenails, it may hurt to wear shoes.
Treatment for nail and skin conditions is often essential to prevent an infection from spreading to other parts of the body and other people.
People who already have another health condition, such as diabetes, should seek prompt treatment if they develop a skin or nail infection, as it is more likely that complications will arise.
Treatment for nail infections
Nail infections can be challenging to resolve.
Dr. Phoebe Rich of the American Academy of Dermatology (AAD) recommends the following three steps to treat Candida of the nails:
- Investigating and resolving any possible underlying medical causes.
- Keeping the nails dry and away from harsh substances or water, for example, by wearing gloves.
- Strengthening the nails with petroleum jelly or thicker-based lubricants rather than watery lotions.
If treatment for a nail infection does not resolve the problem, surgical nail removal may be the best option. A new nail will grow, but it takes time.
Vitamin B with biotin may also help brittle nails. This is a long-term solution that involves taking a daily supplement.
However, the United States Office for Dietary Supplements (ODS) note that more research is necessary to confirm the safety and effectiveness of biotin supplements.
If the condition persists, a specialist may prescribe an oral medication to help with the problem.
Treatment for skin infections
Over-the-counter (OTC) antifungal treatments for the skin include:
- miconazole
- clotrimazole
- oxiconazole
Keeping the skin dry increases the chance of a quick recovery from the infection. This may be more difficult in some regions of the body. Powders can decrease moisture during and after treatment.
When to see a doctor
If the condition does not improve with OTC remedies, it is vital to see a doctor or dermatologist.
Prescription medication may be necessary, or there might be an underlying cause that needs addressing.
The doctor will ask about the person’s medical history and examine any symptoms. For skin infections, they may also take a skin scrape for testing in a laboratory.
They may prescribe:
- a drying agent if necessary, such as miconazole powder
- a topical antifungal agent to apply directly to the skin
Treatment for CMC usually involves a topical antifungal medication, but some people may need a long-term oral medication instead. If an underlying condition is responsible, such as an antibody deficiency, this may require specific treatment.
A Daily Invitation to Breathe Deeply with Cystic Fibrosis.
A possible side effect of nebulizing is a condition known as Oral Thrush (oropharyngeal candidiasis), an infection of yeast fungus in the mucous membranes of the mouth. The aggressor, Candida albicans, is normally present in the mouth, digestive tract, and skin of most healthy people but like many things in life, causes few or no problems until the delicate balance of the chemistry, good bacteria and/or the immune system of the breather is interrupted thus creating a favorable environment for the yeast to overgrow.*
Folks that nebulize daily are, by the nature of how nebulizers deliver medications to patients, putting themselves at risk for disturbing the natural balance of bacteria and chemistry in their mouths. And by the nature of Cystic Fibrosis and CF-related diabetes, patients may have compromised immune systems or potentially increased sugar levels in the saliva = A recipe for yeast overgrowth opportunities.
What Thrush looks like and feels like. Not to be confused with the North America Wood Thrush (bad joke), ORAL Thrush has many levels of severity, and there is plenty of literature to help you pre-diagnose it. So instead of rehashing the info, I am simply going to direct you to here and here. That said, Oral Thrush is generally described as having the following common symptoms:
North American Wood Thrush- Not Oral Thrush
- white lesions on your tongue, inner cheeks, gums, palate, and/or tonsils
- a creamy, white material on the surface of the lesions
- slight bleeding from the lesions when they are scraped
- mouth pain at the site of the lesions
- dry, cracked skin at the corners of your mouth
- difficulty swallowing if the lesions have spread into your esophagus**
- a horse voice and scratchy throat (not necessarily associated with the common cold or flu)
Prevention: Rinse and Gargle! Rinsing your mouth and gargling with water or salt-water after a nebulizer and after taking puffers (especially steroids) is a first line of defense. And limiting the amount of super sweet foods may help too because the food source for yeast is sugar and the more immediately available the sugar is, the more fuel provided to the yeast. (Think basic wine-making theory- winemakers introduce yeast into grape juice to make wine. The yeast will continue to live and make alcohol as long as there is sugar to consume.)
For women who have experienced a vaginal yeast infection before (approx. 75% of all women experience at least one in their lifetime), following the administration of over-the-counter anti-fungal creams, they have probably been instructed to increase their intake of yogurt to introduce good bacteria into their systems because good bacteria may help keep the yeast in check. I recently read that a natural treatment for thrush is eating non-sweetened yogurt but I cannot speak to its efficacy and I have not found much literature on this treatment and this last treatment may offer false promises without more understanding.
Folks over 30 with CF need to lend a serious ear here. Candida is nothing to ignore. As many times as I have been to the doctor in my life, I am not sure if thrush was ever taken more seriously than an annoyance BUT as folks with CF are getting older on average, Candida is posing a more serious problem. Anyone with CF who is 30+ years old should read this paper: “Candida species in cystic fibrosis: A road less travelled”.***
Example of Pastille
Treatment: If a Candida infection is diagnosed in an adult, common medical treatment includes a prescription from your doctor for oral anti-fungals in a pastille or lozenge form. It may be painful to keep up with oral hygiene during a thrush infection, but it is still important. Brushing with a SUPER soft toothbrush with non-abrasive toothpaste and continued rinsing and gargling with salt water is recommended.
Thought to keep in mind: Being a better listener to your body will make you a better communicator on its behalf. Especially for those that nebulize daily, Listen up.
As always, the opinions in this blog post ARE NOT a substitute for medical advice from a licensed and authoritative source. Please consult your health management team (physician, CF Specialist, pulmonologist, respiratory therapist, nutritionist, etc.) for advice on your health management regimen.
What is Oropharyngeal candidiasis?
Candidiasis of the mouth and throat, also known as a “thrush” or oropharyngeal candidiasis (OCP), is a fungal infection that occurs when there is overgrowth of fungus called Candida. Candida is normally found on skin or mucous membranes. However, if the environment inside the mouth or throat becomes imbalanced, Candida can multiply. When this happens, symptoms of thrush appear.
How common is Oropharyngeal candidiasis and who can get it?
Oropharyngeal candidiasis can affect normal newborns, but it occurs more frequently and more severely in people with weakened immune systems, particularly in persons with AIDS.
What are the symptoms of Oropharyngeal candidiasis?
People with Oropharyngeal candidiasis infection usually have painless, white patches in the mouth. Symptoms of Oropharyngeal candidiasis in the oesophagus may include pain and difficulty swallowing.
How do I get Oropharyngeal candidiasis?
Most cases of Oropharyngeal candidiasis are caused by the person’s own Candida organisms which normally live in the mouth or digestive tract. A person has symptoms when overgrowth of Candida organisms occurs.
How is Oropharyngeal candidiasis diagnosed?
Oropharyngeal candidiasis is diagnosed in two ways. A doctor may take a swab or sample of infected tissue and look at it under a microscope. If there is evidence of Candida infection, the sample will be cultured to confirm the diagnosis.
How is Oropharyngeal candidiasis treated?
Prescription treatments such as, Oral fluconazole, clotrimazole troches, or nystatin suspension usually provide effective treatment for Oropharyngeal candidiasis.
What will happen if a person does not seek treatment for a Oropharyngeal candidiasis?
Symptoms, which may be uncomfortable, may persist. In rare cases, invasive candidiasis may occur.
Can Candida-causing Oropharyngeal candidiasis become resistant to treatment?
Overuse of antifungal medications can increase the chance that they will eventually not work (the fungus develops resistance to medications). Therefore, it is important to be sure of the diagnosis from before treating with over-the-counter or other antifungal medications.



